Healthcare-acquired infections (HAI or HCAI) are as common as they are dangerous for patients and occupational staff. They are the cause of numerous post-surgery and post-hospital release deaths. HAI are not present at the time of admission and appear after discharge. This is often due to the contamination of equipment and other medical materials or cross-contamination within the hospital.
Not all microbes are harmful to human health, yet some microbes like bacteria should not be found in the healthcare environments where vulnerable patients are admitted. These microbes also affect medical supplies' durability, causing odours, staining, and damaging materials.
The European Centre for Disease Prevention and Control Centre (ECDC) estimates that 3.8 million people acquire HAI in the European Union (EU) every year. This results in a considerable public health burden, with about 37,000 directly attributable deaths per year and perhaps three times as many partly attributable deaths. The total annual healthcare costs of such infections for the EU were estimated to be 7 billion euros (ECDC 2008), but this probably grossly underestimates direct costs.
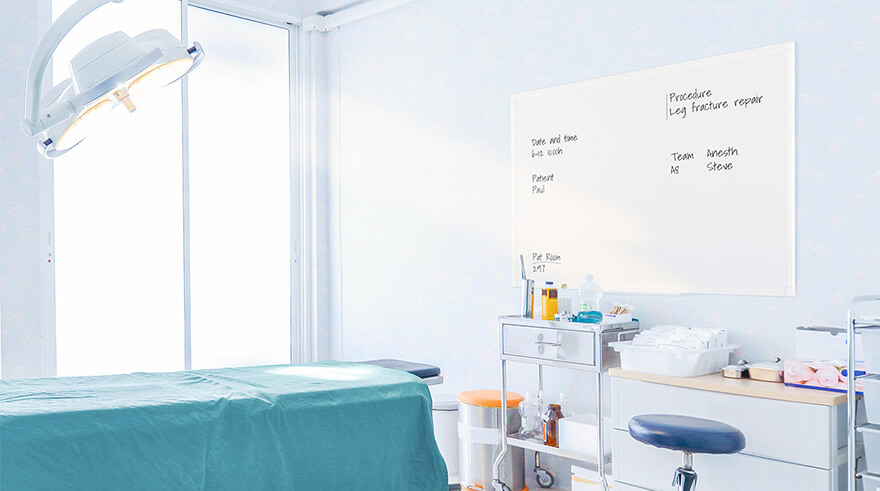
Antimicrobial technology: an extra layer of protection
The healthcare facility's environment affects the patient's overall wellbeing just as the doctor or nurse’s hands. As you enter a patient room in a hospital or primary care physician’s office, you encounter an array of bacteria. Pioneering technologies built into materials used in healthcare settings is a crucial part of keeping these facilities cleaner and safer.
Antimicrobial products have a layer of protection against bacterial growth. They promote hygiene in all environments, especially in healthcare spaces where sanitation is of the utmost importance. Bi-Office designed a collection of Antimicrobial boards that enables safe communication between teams and shifts in those demanding situations.
The Antimicrobial collection integrates BioCote® technology and is proven to greatly reduce bacteria and microbes on protected surfaces. As a result, the potential risk of "surface to surface" or "surface to user" cross-contamination within these surroundings decreases.

Dangerous infections such as Pneumonia, Sepsis, or Multiresistant bacteria can arise from poorly observed cleaning protocols, hand hygiene, or lacking automated disinfection technologies. The trend for public facilities will be to assign antimicrobial products as standards for specific areas of the healthcare building. This guideline will eventually be regarded as critical, following the precedent of mandatory safety regulations like fire prevention, for instance.
Dealing with the Coronavirus threat
The SARS-CoV-2 (COVID-19) pandemic reinforced healthcare services’ need for more extensive disinfection protocols. The protection demands can only be met by incorporating adequate equipment like antimicrobial products, dividers, and hand disinfection dispensers. In addition to these tools, the following sanitary routines must be carried out to prevent cross-contamination and COVID-19 dissemination in medical facilities and senior residences:
- Wash your hands and use a hands-free dispenser to keep them disinfected
- Create an infection-control policy and provide infection control training
- Use gloves for contamination risk tasks and dealing with patients with weakened immune systems
- Provide Personal Protective Equipment (PPE), but also acrylic screens in the reception and waiting rooms, physicians’ offices, and eating areas
- Keep surfaces clean and disinfect them - shared surfaces such as tables, whiteboards, and chairs should have antimicrobial technology to self-clean from contagious bacteria and microbes.
Visit bi-office.com to learn more about the Antimicrobial solutions that keep bacteria away.


.png)